THE growing Asian American and Pacific Islander (AAPI) population in the U.S. is very diverse — encompassing a large number of unique ethnic identities with their own cultures, languages, and experiences.
According to fact tank Pew Research Center, a whopping 20 million Asian Americans trace back to over 20 countries throughout East and Southeast Asia, and the Indian subcontinent. The 19 largest origin groups together account for 94 percent of the total Asian population in the U.S.
Yet despite the population’s vast diversity, AAPIs often get lumped together into one homogeneous group which can be problematic as not all subgroups have the same experiences.
Pew Research Center found, for example, that income inequality in the U.S. to be the greatest among Asians, displacing blacks as the most economically divided ethnic group in the nation.
The same is true in the area of health as not all AAPIs experience health concerns in the exact same way.
When the U.S. Center for Disease Control and Prevention’s (CDC) National Center for Health Statistics in 2016 came out with a study that reported Asian Americans doing better in health than the general population, experts took it as an opportunity to highlight the differences between AAPI subgroups.
For example, while 16 percent of Asian Americans reported having suffered multiple chronic conditions, 24.1 percent of U.S. total did. But when AAPI subgroups were compared with each other, Filipinos reported suffering multiple chronic conditions at a much higher percentage than its Asian counterparts.
Filipino-Americans were found to have reported suffering from multiple chronic conditions such as hypertension, stroke, diabetes, and coronary heart disease at rates higher than other AAPI subgroups. The Fil-Ams’ rate was about doubled that of the Chinese Americans.
Just as it is in areas of economic level and education, AAPIs cannot be lumped into one category when discussing issues of health. But there are health issues that have been found to be of concern across all subgroups, despite affecting them differently.
Cancer, heart disease, and stroke
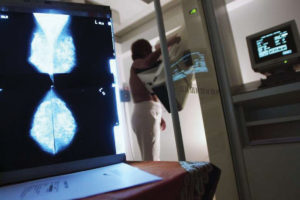
Cancer rates among Asian Americans and Pacific Islanders as a whole are generally lower compared to that of non-Hispanic whites, according to the U.S. Department of Health and Human Services Office of Minority Health (OMH). But as one of the leading causes of death within the AAPI community, there are apparent disparities in the types of cancers.
Compared to non-Hispanic whites, AAPI men are 40 percent less likely to have prostate cancer, but twice as likely to have stomach cancer, according to OMH. Similarly, despite being less likely to have breast cancer than white women, AAPI women were also twice as likely than white women to have stomach cancer.
AAPIs also have the highest occurrence of liver cancer of any racial group in the U.S. The National Cancer Institute found liver cancer to be prevalent in Chinese, Filipino, Korean, Japanese, and Vietnamese populations with rates ranging from 1.7 to 11.3 times higher than white Americans. Vietnamese men had the highest rates.
Heart disease is also among the top concerns for the AAPI community, affecting some groups more than others.
While cancer was a leading cause of death among most AAPI female subgroups, heart disease was the leader among Asian Indian women, according to a study posted in the U.S. National Library of Medicine.
Among men, Asian Indian men also saw heart disease as a leading cause of death. The same was found for Filipino and Japanese men. This, despite cancer showing as a leading cause of death for Asian males when looking at the group as a whole.
The same study listed stroke as the third leading cause of death among almost every Asian subgroup.
Earlier this year, the American i Association found Asian Americans to be more likely than whites to experience a severe ischemic stroke, adding that the findings were a good first step in the direction of looking into subgroups.
Other health issues
While cancer, heart disease, and stroke usually claim the top three spots of health issues for AAPIs, many issues remain on the health radar for all subgroups.
As the issues of mental health awareness gain traction in the U.S., so too has the issue been increasingly discussed in the AAPI community which has often considered the issue a stigma.
The National Latino and Asian American Study found that Asian Americans were three times less likely to seek out mental health services than white Americans.
Reasons for stigma have often stemmed from pressure to succeed or live up to the “model minority” stereotype, family obligations based on cultural values or traditions, and the problem of mental health concerns as simply being considered taboo among others. These issues, in addition to challenges with accessing resources due to language barriers.
The CDC found that in 2014, suicide was the ninth leading cause of death for aggregated Asian Americans, and the 10th for White Americans.
Chronic hepatitis B has also been found to be experienced by many AAPIs. Despite being less five percent of the total U.S. population, AAPIs account for over 50 percent of nearly one million Americans living with chronic hepatitis B, according to the CDC. It adds that at least one-third of Asian Americans living in the state may not know they have chronic hepatitis B.
And while the U.S. population deals with large numbers of those with diabetes and prediabetes, AAPIs too are looking to curb the risk of diabetes.
According to the American Diabetes Association, AAPIs are at an increased risk for type 2 diabetes, compared to white Americans. Unlike other racial or ethnic groups, AAPIs do not have to be overweight to be at risk for diabetes. Furthermore, weight gain poses a greater risk for diabetes among AAPIs compared to other ethnic groups.
Importance of disaggregated data
While the AAPI community has been gaining some recognition as a growing population, it still struggles at times to move past the “model minority” myth, which pits the population as a whole as achieving higher degrees of socioeconomic success and education than the average U.S. population.
When it comes to health, more studies can be made and health experts and advocates hope that through these studies, more understanding of how AAPI subgroups are affected by certain diseases can be achieved.